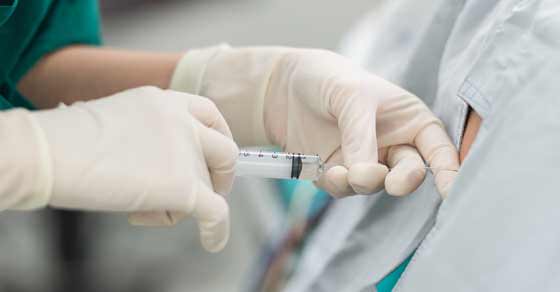
Epidurals during labor are a hot topic. This post is going to talk about the meaning, risks, if it hurts, side effects (both in labor & after the baby), the procedure and other alternative pain meds you can use during labor.
**As always please take the advice of your physician over any advice on my blog (or frankly, anywhere on the internet). They know your personal circumstances and health history and can help you make the best choice for you.**
First off, hello! I’m Hilary — many people know me as The Pregnancy Nurse 👩⚕️. I have been a nurse since 1997 and I have 20 years of OB nursing experience, I am also the curly head behind this website Pulling Curls and The Online Prenatal Class for Couples. 🩺 I’ve helped with THOUSANDS of epidurals, so I think I’m a good resource for this one!
I am SUPER excited to give you correct and useful info on epidurals as there is a LOT of info out there (and a lot of it is wrong).
Epidurals are something that there are TONS of questions about — I even created a podcast on it.
And, if you’re this interested in epidurals make SURE you’re ready with your hospital bag too with my hospital bag checklist:
Alright, let’s talk about epidurals!
Epidural During Labor
Why get an epidural in labor?
An epidural during labor is given to help with the pain. It numbs the nerves from about your bra level to your knees. The plan is for about 80% of the pain to be taken away with the epidural. Want to know more about how much pain to expect, read my other post — does labor still hurt with an epidural?
You will still feel pressure.
And, you should still be able to move in your bed to promote the labor process and be able to push.
Most often, any more in the US. The Epidural is placed and “bolused” (that means they give a large amount of medication at once).
The anesthesiologist puts in a tube into the epidural space. Then, it is placed on a pump that drips in medication until you have your baby or we turn it off.
What is an epidural block?
An epidural goes into the epidural space. Your brain and spinal column are covered by several membranes. They go between two of those in the “epidural space”. You can see more about it here.
One doctor said it’s like a banana, and you’re trying to slip the medicine between the peel and the banana — which is a pretty good metaphor.
The epidural space is before your spinal cord, so the needle is not going in the same space that holds your spinal column. Just so you know (I know a lot of people worry about that).
It is, however, still near your spinal cord and sometimes it can brush up against nerves as they thread the tube in to make it last.
Want to know more about the actual epidural process? I go through it step by step with a Raggedy Ann doll in here that makes it super easy to understand, and not scary!
Epidural Side Effects during labor
One of the “side effects” is the numbness and your legs feeling very heavy.
Other common side effects can be itching or your blood pressure falling (which is why your nurse gives you a lot of fluid in your IV before the epidural). Some people also experience nausea (which we can give medications to help).
Some people also experience nausea & itching.
Studies show that it can prolong the pushing phase of labor, although it is hard to know if those studies are taking into account the fact that often we let you “labor down” when you are comfortable. That means you relax and let your baby come down with your uterus and then when it is lower, you start to push, effectively decreasing the amount of time you push.
Women without an epidural often can’t let the baby “labor down” because they feel too strong of an urge to push.
Epidural side effects after birth
The most common long-term side effect is back pain — like a bruise in the area. I notice for about 10 days I feel pain when water hits it in the shower. Similar to the bruise from the IV.
A few people have complained of long-term back pain after an epidural, and I have a whole post on back pain after the epidural you might find helpful.
Having a baby is rough on your back. All the sitting/feeding, picking the baby up, handling the car seat — studies show that likely causes the longer-term back pain.
Epidural Risks
Your anesthesiologist should go over this (and many others) before placing it — called informed consent.
The most common risk is a spinal headache (which is due to a small amount of spinal fluid leaking out). They can do a “blood patch” to help with it. It happens in about one in 100-200 epidural placements.
Of course, with all elective treatments where the skin is broken, there are risks of infection.
And, like all good informed consents, there is always the possibility of paralysis or death.
That risk is very small — extremely rare — but be aware that a true informed consent requires mentioning it. Just know that, so when they mention in it — you’re not thrown off guard.
In all my years of doing L&D I have neither seen nor heard of any patient having paralysis or death from an epidural.
Some people mention a risk of a fever, but often your temperature does go up (below 100 degrees) while the epidural is in place. That would not be considered a fever as it’s still so low, and is likely caused by the cool fluid so near to the spinal nerves.
The Epidural and Being Afraid of Needles:
First off, no one loves needles, not even nurses.
The main good news is that you will likely not see the epidural needle. Most women are in enough pain and are just listening to the guidance of the anesthesiologist that they can pretty easily get over that and get an epidural.
It is humanly impossible to see the epidural placed…. due to positioning.
Before we keep going, I gotta ask if you’re doing your kick counts? They are your best indicator of fetal well-being. Most people do them wrong, so I have a cheat sheet right here:
Epidural Pros and Cons
Pros
- It takes away the pain
- It makes vaginal exams less painful
- It can lessen the urge to push so you can “labor down” instead of pushing longer
- It numbs your vagina/perineum in case of a tear
- If you had to have an emergency cesarean, they can numb you through the epidural
- Allows you to get some rest
- It allows you to concentrate during crowning to allow the tissues to stretch
Cons
- You aren’t able to move around as much
- It can lessen the urge to push which can make pushing time longer
- No walking/using the tub
- It only takes away 80% of the pain and some people find that to be still too much
- It sometimes doesn’t work and you have to have it replaced
- Some patients have a “window” that can’t be numbed.
- Epidurals are associated with a higher c-section rate (but that can be due to a variety of factors — so talk to your doctor if you have questions about that)
- You do have to stay still for them to put it in.
- Sometimes they don’t work.
- You have to have a urinary catheter as you can’t get up to the restroom (that’s a tube that goes up to your bladder to drain out your urine — it is removed before/following delivery)
There is a lot of crazy information out there about epidurals, so make sure when you’re taking information about epidurals you’re doing it from someone who is up to date with the research and has a lot of experience about them. Experience in birth education is SO important.
Epidural Anesthesia Procedure
The basic process looks like this
**The epidural is placed by an anesthesiologist or a nurse anesthetist, not your OB**
- You sit on the edge of the bed (some doctors also do it side-lying)
- Curl around your baby (think of a mad cat, or a boiled shrimp)
- The Doctor will prep the area with special soaps to keep it all clean (that area is now considered sterile, so you want to be sure to not move too much or touch it) and place a drape over the area
- The doctor numbs the skin area (I have a post on if an epidural hurts)
- He inserts the needle
- He moves the needle with very tiny movements to find the right space
- He injects a little fluid
- He injects a test dose to make sure he’s not in a blood vessel
- He inserts the catheter (In the hospital tubes are called cathers, this one goes into that space and is about as wide as a piece of thin spaghetti) so the medicine can continue to go in
- He gives you a “bolus dose” (a large amount of medicine that will help to get you numb faster)
- He secures it with tape.
This usually all takes 20-30 minutes, and most patients are finding comfort within 20-30 minutes of the bolus dose.
And, like I said before we go through the whole process together in here to make it easy to understand and not scary.
Epidural Drugs
It can be given in a variety of ways, each doctor has their own mixture they use.
In my hospital, we currently use bupivacaine and fentanyl.
But again, each hospital and doctor are different.
The epidural medication is most often pumped in until you have your baby. It is like a small IV pump that continually replaces it.
So, the epidural should not wear off before you have your baby. However, in rare cases, the catheter migrates and it no longer works. I have a whole post about how long epidurals last.
Alternatives to the Epidural
I talk about all the options in my post on pain management during labor.
A few final thoughts about the epidural
- Anesthesiologists can often be tied up doing other things, so if you are considering it, let your nurse know. That way she can get you “in line” or between c-sections.
- Most often, only one other person can be in the room during an epidural placement, and most practitioners prefer they sit in front of mom.
- If you feel like it’s not working, the only one who can truly fix it is the anesthesiologist. Ask to see him/her. Remember that sometimes the only fix is to put it in again.
- The epidural is secured with a large amount of tape, so you can still move in bed, but be thoughtful of dragging your back across the bed if possible.
- Before a cesarean section, patients are given a spinal. The difference is the area where they put the medicine. However, most often an epidural can be used if you already have one in place. Learn more about the epidural vs the spinal.
Epidurals are great and can take away a lot of the pain of labor, but I recommend having some pain coping skills to utilize before an epidural (if that is your plan). I have a whole post on increasing your chances of a natural delivery that you might like to read.
If you have more questions before it is placed, you can always talk to an anesthesiologist before you are admitted, or your OB doctor might be able to answer the simpler questions as well.
So, that’s the nitty gritty on the placement of an epidural. Just a reminder this is part of a series on labor epidurals. don’t miss the other two:
- Does labor still hurt with an epidural?
- Does it hurt to get an epidural?
- How Long Does an Epidural Last?
Epidurals are complicated, and they can seem really scary.
And frankly, a lot of birth can seem scary too. But I really don’t think it needs to. The Online Prenatal Class for Couples has proven to decrease patient’s anxiety by over 60% — wouldn’t it be nice to feel prepared instead of scared:
- No surprises from the epidural process, you’ll know it like a pro
- Know WHEN to get your epidural during labor (or maybe if you don’t even need it)
- Loads of natural pain management techniques to get you through labor or to the epidural if you want.
Or, if you’re not quite ready for the full class, check out my free prenatal class — It’s your first step towards being your own birth boss.













Kristie says
OMG! I understand that you are giving the facts about epidurals, but my goodness you made it sound like the scariest thing ever. I have had epidurals for both of my births and they weren’t that scary or that bad. It’s good that you are giving women the bottoms line of epidurals but geez. Lol
Hilary Erickson says
Nope, they shouldn’t be NEAR that scary. 🙂
Kate says
Whew, I’m glad I have had both my babies all natural. I would rather push with pain than have that in my back! I’ve needed an IV both times because of strepB, but I could still walk around right up to the pushing stage. I’m glad the epidural is there for those who so desire, but not for me.
Hilary Erickson says
Yup, — it’s nice that there’s all sorts of options. 🙂
Betheaces says
This article is really great! Awesome job!
Hilary Erickson says
Awh, thank you!
Liz says
I’m so thankful I ran across your article! I’m due in November with my suprise baby, I have two teenagers and I’ve forgotten just everything! Thanks for the great info!!
Hilary Erickson says
So glad! Might want to consider our full class too! So many second (or more) time moms are loving it!
RMama says
I had a spinal block with first and every day after that for about a year my legs would go numb immediately if I would lie on my side (either side). I had an epidural with my second for fear of a repeat c section and my anesthesiologist was very good and I only had minor bruising and numb spells for a few weeks. Honestly, I didn’t have any issues except I couldn’t feel enough to know when to push and so I just pushed. My second was born in three pushes and I feel like because of my position and not being able to feel. I had my 3rd degree tear.
Hilary Erickson says
The numbness is definitely not normal, so I’d check with your provider.